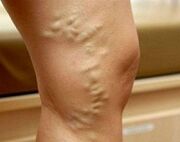
Varicose veins during pregnancyis an ectasia of venous vessels that arose in the gestational period and is pathogenetically associated with it. It is manifested by severity, paresthesia, pain in the lower extremities and external genitals, swelling, muscle twitching, trophic skin lesions. It is diagnosed by examination, ultrasound angioscanning methods. During pregnancy, treatment is usually limited to compression therapy with correction of sleep and rest, physical activity, and nutrition. Perhaps the appointment of phlebotonics, phleboprotectors, anticoagulants, antiplatelet agents. Surgical treatments are usually used after childbirth.
General information
Varicose veins (varicose veins) are one of the most common vascular diseases associated with the gestational period. According to studies, up to 15-20% of people suffer from venous pathology, while 2/3 of them are women, and 60-80% of venous ectasia cases have arisen due to pregnancy. The disease is usually diagnosed for the first time in young patients, 75% of whom are under the age of 30. In more than two-thirds of cases, the clinic of varicose veins debuts after the 20th week of the first pregnancy. The relevance of timely diagnosis of varicose veins is associated with a high probability of fetoplacental insufficiency and the risk of fatal thromboembolic complications in the absence of adequate therapy.
Reasons
Taking into account the statistical data on the frequency of varicose veins during gestation, most specialists in the field of obstetrics and gynecology consider the disease as a complication of pregnancy. The predisposing factor causing vascular ectasia in 91% of patients is a genetically determined failure of the middle vein sheath, in which the amount of collagen substance is reduced and the content of polysaccharides is increased. The development of varicose veins in constitutionally predisposed women during pregnancy is facilitated by:
- Increased circulating blood volume. The increase in the BCC in pregnant women ranges from 30-50% (when carrying 1 child) to 45-70% (if there are 2 or more fetuses in the uterus). This compensatory mechanism allows to ensure adequate blood supply to the child, the vital organs of the woman and the fetoplacental system.
- Hormonal changes during pregnancy. During gestation, the ovaries and placenta intensively secrete progesterone and relaxin. Under the influence of these hormones, the smooth muscle fibers of the veins relax, and the structural reconstruction of the connective tissue occurs. As a result, the vascular wall copes worse with the increased intravenous pressure.
- Compression of vessels by the pregnant uterus. The growing uterus compresses the inferior vena cava and iliac veins. The outflow of blood from the pelvis and lower extremities is impaired, intravascular pressure increases, which provokes stretching of the venous walls. The influence of this factor plays a key role in the formation of varicose veins after the 25th week of pregnancy.
- Changes in the hemostasis system. As labor approaches, the fibrinolytic activity of the blood decreases, and the number of coagulation factors increases. This adaptation mechanism is aimed at reducing the volume of physiological blood loss during labor. This increases the likelihood of thrombosis of pathologically altered veins.
An additional etiofactor contributing to the onset of varicose veins in pregnant women is a decrease in physical activity. With insufficient work of skeletal muscles, blood stagnation in the legs and pelvis increases. The situation is aggravated in the presence of excess body weight, in which there is an even greater increase in the volume of blood circulating in the patient's vascular bed.
Pathogenesis
The starting point in the development of varicose veins during pregnancy is the disruption of the compensatory capabilities of the valve apparatus of the venous network. Due to an increase in the BCC and mechanical obstruction to the outflow from the lower extremities, when the main veins are squeezed, the blood exerts increased pressure on the vascular wall. Genetically inherited connective tissue fiber failure is enhanced by the relaxation of vascular smooth muscle under the action of progesterone. As a result, the lumen of the vein expands, the valves stop closing, blood is deposited in the vascular system of the lower extremities. As the disease develops, the pathological process can spread to the vessels of the vulvar ring, vagina, and small pelvis.
Classification
The main criteria for systematizing the forms of varicose veins are the anatomical prevalence of venous stasis and the severity of the disease. This approach allows for a differentiated selection of treatment regimens for different variants of the disorder. Taking into account the involvement of various organs in the process, varicose veins of the lower extremities, vulvar varicose veins, varicose veins of the pelvic organs are distinguished. According to the severity of clinical symptoms, the following stages of expansion of the venous vessels of the lower extremities are distinguished:
- Compensated varicose veins. There are no external signs of vascular ectasia, the pregnant woman notes fatigue of the legs by the end of the day, discomfort in the calf muscles during exercise and brisk walking.
- Subcompensated varicose veins. A vascular pattern ("stars") appears on the skin. In the evening, the legs swell, at night there are cramps, numbness, pain. Bruises and scratches heal longer than usual.
- Decompensated varicose veins. The patient is constantly worried about pain in the legs, swelling is increasing. The veins are markedly enlarged, knotty. The skin is hyperpigmented. There are signs of eczema and trophic disorders.
With pelvic varicose veins in pregnant women, the disease also develops in stages. At the first stage, the diameter of the affected vessels in any venous plexus of the pelvis does not exceed 5. 0 mm. With the second, the uterus or ovaries are involved in the process, the lumen of the vessels is 6. 0-10. 0 mm. The third is characterized by ectasia of veins of more than 10 mm with total involvement of all pelvic venous plexuses.
Symptoms of varicose veins
In 80-82% of patients, the disease debuts with a feeling of heaviness, tension, "buzzing" in the legs, increasing in the evening and during physical exertion. The symptomatology of varicose veins increases gradually. As the disease progresses in some areas of the muscles, pain arises, which first develops with prolonged standing, performing physical work. In the most severe cases, the pain becomes constant, and its intensity can be so pronounced that the pregnant woman experiences difficulties in independent movement. Up to 60% of patients note cramps of the calf muscles, up to 40-50% - loss of sensitivity, numbness of the legs, up to 30% - itching.
At the subcompensated stage of varicose veins, external signs of expansion of superficial veins appear. First, areas of reticular vessels and telangiectasias ("reticules" and "stars") are formed on the skin. Subsequently, the venous pattern becomes distinct. Veins look dilated, convoluted, eventually nodular. The spread of the process of ectasia to deep vessels is evidenced by the occurrence of edema in the ankle joints and lower legs. With decompensation of varicose veins, the skin of the legs looks hyperpigmented, eczema develops. If the pathology arose long before pregnancy, dystrophy of the subcutaneous fatty tissue, trophic ulcers is possible.
In 4% of patients, the disease affects the veins of the vulva, vagina, and small pelvis. With vulvar and vaginal varicose veins, discomfort, distention, heaviness, itching are observed in the area of the external genitals. There may be swelling of the perineum and labia, contact bleeding from the vagina after sex. Pelvic congestion syndrome is manifested by pulling or aching pains in the lower abdomen, which radiate to the lower back, sacrum, groin, and external genitalia. Dyspareunia (soreness during intercourse) is characteristic. In severe cases, dysuric disorders are detected.
Complications
In the absence of adequate treatment, varicose veins in pregnant women can be complicated by the development of trophic ulcers, erysipelas, thrombophlebitis, thrombosis of superficial and deep veins, thromboembolism of the pulmonary artery and other great vessels during labor. In 40-45% of cases, placental insufficiency occurs with acute and chronic fetal hypoxia. In 25% of patients, abnormalities of labor are observed (weakness of labor forces, discoordination of the contractile activity of the myometrium). With vaginal varicose veins, massive traumatic course of the postpartum period is possible. Almost a third of women in labor have defects in the separation of the placenta and discharge of the placenta. The long-term consequences of varicose veins that have arisen during pregnancy are hemorrhoids, disabling chronic venous insufficiency, and pelvic pain.
Diagnostics
With the appearance of characteristic skin signs, the diagnosis of varicose veins during pregnancy usually does not present any difficulties. The tasks of the diagnostic stage are to determine the stage and localization of venous ectasia, to exclude other causes that can cause stagnation in the vasculature of the lower extremities. The most informative survey methods are:
- Chair Inspection. The study reveals characteristic changes in venous vessels in the vulvar region and on the inner thighs - ectasia, tortuosity, nodosity. Swelling of the labia and perineum is possible. When viewed in the mirrors, the vaginal mucosa looks hypertrophied, cyanotic. Vaginal vaults with bimanual palpation are smoothed, often painful.
- USDG of the venous system. During ultrasound scanning, the shape and diameter of the vessels, their length, anatomical position, and the condition of the wall are assessed. The method allows you to determine the zones of branching, the consistency of the valve apparatus, the patency of the veins, the presence and direction of reflux. It is possible to scan both the vessels of the lower extremities and the inferior vena cava (IVC ultrasound).
- Duplex scanning of leg vessels. The advantage of the non-invasive method, which combines traditional ultrasound and Doppler studies, is not only obtaining detailed information about blood flow parameters, but also visualization of the venous network. Duplex angioscanning is used for a comprehensive assessment of the state of superficial, perforating and deep vessels.
Radiodiagnostic methods (varicography, selective ovarycography, ascending phlebography of the extremities, pelvic phlebography, CT venography, phleboscintigraphy, etc. ) during pregnancy are used to a limited extent due to a possible negative effect on the fetus. In difficult cases, with suspicion of pelvic varicose veins, diagnostic laparoscopy is performed with caution. Differential diagnosis of varicose veins of the legs is carried out with dropsy of pregnant women, heart failure, lymphedema, acute thrombosis of the venous system. Varicose veins of the small pelvis must be differentiated from genital endometriosis, chronic inflammatory pathology of the pelvic organs, submucous and subserous uterine myomas, cysts and other ovarian tumors. In addition to the observation of an obstetrician-gynecologist, the patient is recommended to consult a phlebologist, cardiologist, and oncologist.
Treatment of varicose veins during pregnancy
The main objectives of therapy for varicose veins in pregnant women are to stop the progression of the disorder, mitigate the severity of the clinical picture and prevent possible thromboembolic complications. Non-pharmacological methods are considered preferable, if necessary supplemented with pharmacotherapy in safe stages of pregnancy:
- Compression therapy. A woman with a confirmed diagnosis of varicose veins is recommended to wear it daily throughout pregnancy, to use elastic bandages, special compression tights or stockings of 1-2 compression class during childbirth and the postpartum period. Compression treatment by mechanically reducing the diameter of the superficial veins accelerates blood flow, reduces swelling and congestion.
- Herbal phlebotonics and phleboprotectors. The effect of the use of drugs of this group is associated with an increase in the tone of the venous wall, a decrease in its permeability, an improvement in microcirculation, rheological properties of blood and lymph outflow. The advantage of most bioflavonoids is that they can be used during pregnancy and lactation. Phlebotonic medicines are prescribed both in tablet form and externally.
- Anticoagulants and antiplatelet agents. In the presence of signs indicating a tendency to increased coagulation and the threat of developing DIC, drugs with antithrombotic activity are used with caution. To improve the rheology of blood and vascular microcirculation, pharmaceutical agents are shown that prevent platelet aggregation and have an angioprotective effect.
Pregnant women with varicose veins are recommended special complexes of physiotherapy exercises, lymphatic drainage massage, dosed walking, daily ascending contrast shower. Diet correction involves the consumption of foods rich in fiber and vegetable fats. Injection sclerotherapy, miniflebectomy, crossectomy, endovasal laser coagulation and other surgical methods of treatment are used in exceptional cases with severe forms of the disease, severe pain syndrome, and the presence of complications. Most often, surgical correction is carried out at the end of the lactation period.
Delivery tactics
The preferred method of delivery for varicose veins is natural childbirth, at the beginning of which elastic bandages or compression garments are applied to the woman's lower limbs. Patients with vulvar-vaginal varicose veins require especially careful maintenance of the persistent period with the performance of a protective perineotomy according to indications. When ectasized veins rupture, the damaged vessels are carefully ligated with repeated stitching of the conglomerate of nodes. Cesarean section is recommended for patients at high risk of thromboembolic complications and severe vulvar varicose veins.
Forecast and prevention
With timely detection and adequate therapy, the prognosis is favorable. For prophylactic purposes, it is recommended to have sufficient night's sleep and periodic rest throughout the day in the supine position with the legs laid on a firm surface at an angle of 30 °. Pregnant women with a burdened heredity should refuse to wear shoes with heels of more than 5 cm, limit the duration of sitting or standing, and control weight gain.
To prevent varicose veins, daily walking, reducing salt intake, taking vitamin preparations that strengthen the vascular wall are effective. Patients with varicose veins planning a pregnancy, according to indications, undergo surgical interventions to correct the disease.












































