Varicose veins, more commonly known as varicose veins, occur when the veins stretch and enlarge, taking on a blue-purple or red hue, due to the accumulation of large amounts of blood. This is a widespread disorder that most commonly affects the legs (most commonly the calf muscles), but can also develop elsewhere.
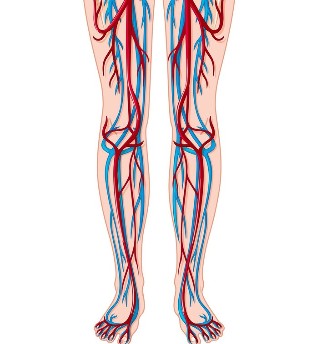
In general, the blood supply to cells, known from the course of biology, occurs as follows: from the left ventricle of the heart, oxygen-enriched blood through the aorta enters the arteries and from there into the smaller blood vessels up to the capillaries, with the help of which the organs and tissues of the body receive oxygen and the substances they need. . . The blood is then collected from the capillaries through small blood vessels called “venules, ” and transported into larger veins, whose task is to direct the blood back to the lungs and heart in order to be oxygenated and repeat its way. The mechanism for directing blood to the heart is called a venous pump.
Veins are blood vessels that return blood from body tissues to the heart.
Some veins have one-way valves that open to allow blood to flow to the heart and close to prevent backward blood flow.
Actually, this is how varicose veins turn out: if the valves are damaged and do not block the flow of blood, it accumulates in the veins, which causes them to swell and stretch, which leads to varicose veins. Angiosurgeons claim that varicose veins are such a pathological process as a result of which a change in the venous wall occurs, followed by valve insufficiency.
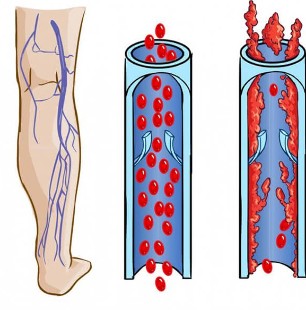
Varicose veins create a return flow (reflux) of blood due to valve dysfunctions. They do not close the vein cavity, which makes it possible for blood to flow in the opposite direction. As a result, an increased venous blood pressure is created, which violates the integrity of the vein walls - they expand and protrude under the skin.
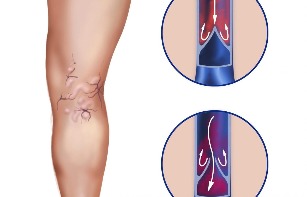
Since varicose veins are a modification of veins, pathology is ranked not only as vascular diseases, but also as cosmetic problems. Normal veins and varicose veins - when there is reverse blood flow and varicose veins due to valve malfunction.
Why are the legs most often affected by varicose veins?
There are 3 types of veins in our legs - superficial veins that are closest to the skin; deep veins, which are located inside the muscles and connect to the largest vein in our body - the vena cava leading to the heart; and perforating veins, connecting superficial and deep veins. The varicose veins that we see occurs precisely in the superficial veins closest to the skin.
When we are upright, the blood in our legs should be directed up to the heart, resisting the pull. To do this, the muscles of the legs contract and press on the deep veins, pushing blood towards the heart. When the muscles in the legs contract, the valves inside the veins open; when the muscles are relaxed, the valves close, blocking the flow of blood towards the feet.
As you may have guessed, varicose veins are more common in the legs because the pressure of gravity, which increases while sitting and standing, has the greatest effect on venous circulation in the lower extremities.
How dangerous are varicose veins
For most people, varicose veins are, first of all, an aesthetic problem, and at first they do not pose a threat to health. Swollen, ugly veins can spoil the appearance of certain areas of the body, but in most cases they do not impair blood circulation. At the same time, it is noted that if you do not pay proper attention to the fight against varicose veins, its appearance deteriorates over time and complications may develop.
Causes of varicose veins
A number of factors can increase your risk of developing varicose veins:
- Factor # 1 - heredity. If anyone in your family has or has varicose veins, you are more likely to inherit it.
- Gender. Varicose veins are more common in women than in men.
- Age. As we age, our veins and valves become weaker.
- Disruption of blood flow between arteries and veins.
- Hormonal changes. Hormonal changes during pregnancy, premenstrual period and menopause increase the risk of varicose veins. During pregnancy, the growing fetus presses on the veins in the legs. Varicose veins that appear during this period become less noticeable after 3-12 months after the birth of the child. Moreover, each subsequent pregnancy increases the risk of varicose veins.
- Overweight or obese. The extra weight puts a lot of pressure on the veins, which can lead to varicose veins.
- Sedentary and standing work and a sedentary lifestyle. If you stand or sit for a long time, you increase the risk of varicose veins. This is because it is more difficult for the veins to deliver blood to the heart during prolonged immobility.
Symptoms of the development of varicose veins
In addition to the appearance of protruding dark blue or purple veins, here are the main signs of developing varicose veins:
- Slight swelling of the ankles and feet, especially after standing for a long time.
- Pain, burning and heavy legs.
- Leg cramps and throbbing.
- Itching in the ankles and lower legs, often misdiagnosed as dry skin.
- Changes in skin color in the area of varicose veins (bruising).
How to prevent varicose veins
According to specialists from the Department of Surgery at the University of California, the first thing a person can do to prevent varicose veins is to change their lifestyle with the introduction of new habits. These same changes, although they will not help get rid of the already formed varicose veins, will reduce the likelihood of deterioration in its appearance, as well as reduce pain and save other parts of the veins from the formation of varicose veins.
What needs to be done in order to reduce the likelihood of varicose veins or to protect already affected veins from worsening:
- Do not sit or stand in one place for long periods of time. Try to move at least every 30 minutes.
- When sitting, don't cross one leg.
- Raise your legs if possible when sitting or lying down. Try to raise your legs so that they are above the level of your heart.
- Exercise. This will move the muscles in your legs and channel the blood through your veins more efficiently.
- If you are overweight, try to get it back to normal. This will help improve circulation and reduce stress on the veins.
- Avoid tight-fitting clothing, especially around the waist, hips, and legs.
- Don't wear high heels too often or for too long. Low-heeled shoes help to tone the calf muscles, making it easier for blood to flow through the veins.
- Exercise regularly. This will help improve blood circulation, shed extra pounds and maintain a healthy weight.
Complications of varicose veins
According to the position of the Circulatory Foundation, although varicose veins deteriorate over time, this process takes a very long time. It is also noted that in some people who have encountered varicose veins, high pressure in the veins can damage the skin in the ankle area and change its color, as well as the appearance of white scars.
If untreated, progressive varicose veins can lead to more serious negative consequences:
- The appearance of ulcers
- Phlebitis
- Bleeding
- Deep Vein Thrombosis (DVT)
If a person develops eczema (a red skin rash), it may subsequently progress to ulcers that need to be surgically removed.
Phlebitis is an inflammation of a vein that is often accompanied by a thrombosis within the affected vein that becomes hard but fragile. In most cases, this disorder does not pose a serious health risk, although it is often mistakenly confused with the more serious pathology of deep vein thrombosis (DVT).
Many people fear that an accidental blow of a varicose vein will bleed it, but this is very rare. If this happens, then the blood is stopped by applying a tight gauze bandage and applying ice. The person needs to lie down so that the legs are higher than the heart, and, without putting it on the back burner, seek medical help so that specialists can perform procedures that reduce the risk of re-bleeding.
Some patients suffering from varicose veins later face another pathology - deep vein thrombosis. It is not fully known to science whether varicose veins directly increase the risk of DVT. The symptoms of DVT are swelling and pain, and skin that is hot to the touch. Deep vein thrombosis mainly affects the large veins in the thigh and calf muscles, according to experts from the US National Library of Medicine, while it is noted that almost always TRV develops in only one leg.
Varicose veins treatment
Compression therapy
When the first symptoms of varicose veins appear, it is recommended to wear compression clothing. Stockings, tights, or leggings apply light pressure from the bottom of the leg upward, reducing blood build-up and reducing swelling. In this case, the effect is achieved only if you wear them regularly. While wearing compression stockings will not cure existing varicose veins, it will help prevent or reduce varicose veins and further complications.
In addition, the Society for Vascular Surgery (SVS) in its clinical guidelines for the treatment of patients with varicose veins of the lower extremities and pelvis notes: "Wearing stockings is the first therapeutic procedure for patients who have had ulcers removed during the progression of varicose veins. "
Endovenous ablation (radiofrequency or laser)
Endovenous ablation uses laser or radiofrequency therapy to close or remove the varicose vein. The doctor makes a tiny incision in the skin near the vein and inserts a catheter into it. After that, a special device is connected to the tip of the catheter, with the help of which the catheter heats up and closes or removes the varicose vein (depending on the chosen ablation method). The procedure is performed using local anesthesia and the patient usually returns home the same day.
Endovenous ablation is one of the most effective and safest treatments for varicose veins. The Society for Vascular Surgery (SVS) recommends that this procedure be preferred over the surgical method for treating superficial varicose veins.
Sclerotherapy
This is another gentle method of treating varicose veins. During the procedure, a special substance is injected into the vein affected by varicose veins, which destroys the inner lining of the vein and causes blood to coagulate inside it. Over time, the vein collapses and disappears.
Surgical method
In advanced cases of varicose veins, more gentle treatments will not help to correct the situation. In this case, the person is referred for an operation, during which the superficial vein is surgically removed. The indications for surgery are:
- Ulcers or the threat of their appearance,
- Bleeding,
- Phlebitis.
The procedure is performed under general anesthesia, and the patient is usually allowed to go home on the same day. For 2 weeks after surgery, a person may feel pain and discomfort.
The Blood Circulation Fund notes that sometimes deep vein thrombosis may develop after surgery, but the risk of this pathology can be reduced by wearing compression stockings and maintaining high motor activity.
Varicose veins and training
A lot of movement and moderate exercise are the main helpers in the fight against varicose veins.

However, while some training methods are helpful and recommended as prevention of varicose veins, others can be harmful.
Moderate, rhythmic physical activity (such as walking) positively contributes to preventing varicose veins and helps to minimize the likelihood of complications, as dynamic muscle movements help direct blood from the periphery to the heart.
Walking
Walking is one of the best movements for varicose veins prevention and promotes healthy circulation by stretching and contracting the venous pump in the calf muscles. Walk for at least 30 minutes at least 5 times a week.
Low-intensity running
Running at a low pace works well for the calf muscles, but it has one drawback - running puts stress on our joints. If you are not ready to replace running with another activity, run on grass or rubberized paths, not on hard asphalt.
Elliptical & Exercise Bike
Elliptical trainer and stationary bike workouts actively engage the calf muscles, promoting healthy circulation. It also puts less stress on the joints than running.
Strength training
People with varicose veins should avoid excessive amounts of very intense resistance training. During prolonged muscle tension of an irregular nature, the muscles of the legs and ventilator pumps do not contribute to the return of blood to the heart through the veins. For this reason, during exercise, blood accumulates in the veins of the legs, which can only contribute to the further development of varicose veins. In addition, the increase in intra-abdominal pressure during straining also impedes blood circulation.
Squats, lunges, and crunches are particularly noted among exercises that negatively affect venous circulation.
People with varicose veins need to train lightly and do relatively high repetitions in sets without going to failure. In addition, pedaling on a stationary bike or exercising on an elliptical trainer is recommended to restore normal circulation after strength training. It is also recommended to wear compression stockings during and after strength training.
Why veins bulge more in summer

As noted by experts from the V. I. St. John and the Hospital. Saint Joseph Wayne, in the summer the veins bulge more due to the fact that under the influence of heat they expand and fill with more blood, increasing in size.
In order to reduce vein swelling during the summer, follow these simple guidelines:
- Lubricate skin with a thick layer of moisturizing SPF cream.
- If you are outdoors for a long time, try to hide in the shade.
- Don't sunbathe for too long.
- Swim regularly. This way you will carry out cooling procedures for your body, preventing the veins from growing in size.
- Try to wear flats / low-cut shoes and sandals rather than high-heeled shoes.
- Drink plenty of fluids.
You shouldn't start the situation, you need to take action right away.












































